Unlocking the Mystery of Saddle Bone Deformity: Causes, Treatment, and Prevention
Do you often feel a sharp, burning sensation at the top of your foot? Is there a visible bump that’s causing discomfort in your daily life? It could very well be a ‘saddle bone deformity.’ Let me assure you, it’s not as daunting as it sounds. Today, we’re about to set out on a journey to unravel this medical mystery and help you carry forward with ease.
Understanding Saddle Bone Deformity
Saddle bone deformity is a condition of the pelvis that causes one or more of the bones in this area to be malformed. The result is an abnormal alignment, which can cause pain and discomfort. Saddle bone deformities may also affect your ability to move around, making it difficult for you to stand up straight or walk without feeling pain in your hips or lower back.
If left untreated, saddle bone deformity has been shown to worsen over time; however, there are treatments available that will help alleviate symptoms so that you can live life without worrying about how they’ll affect your quality of life–or even worse: lead an active lifestyle!
What is Saddle Bone Deformity?
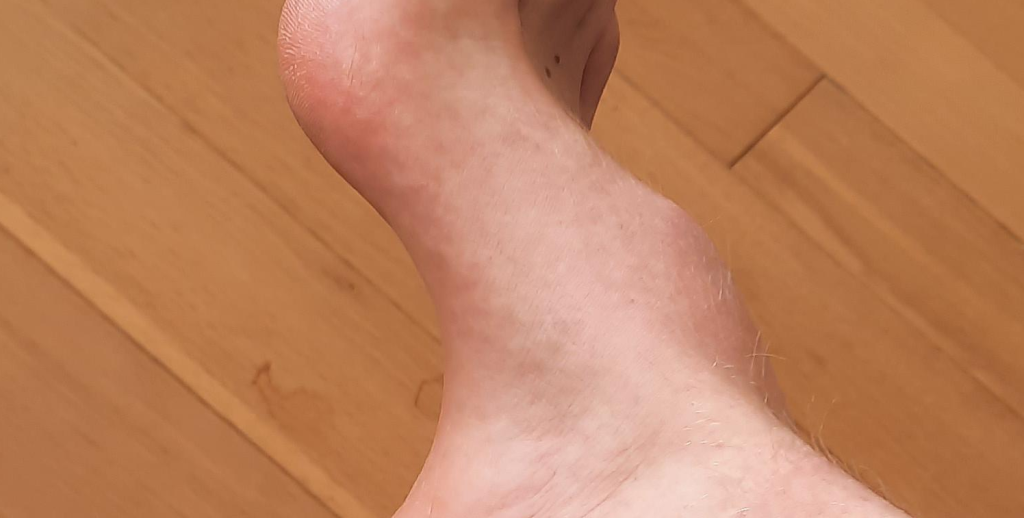
(Source:Reddit)
Saddle bone is a small, triangular shaped bone that sits just below the kneecap and connects it to your shinbone. It’s also known as patella, which means “little plate” in Latin.
The saddle bone can be injured during sports activities like running or jumping, but it’s most commonly injured by falling on hard surfaces like concrete or asphalt while walking or running.
Relation with Exostosis
Deformity of the saddle bone is a common condition that can be caused by many things. One of them, however, is exostosis.
Exostosis is a bony growth that forms on the outside of your body and usually causes no pain at all. However, if you experience any pain in your hip or groin area, it could be due to this condition as well as saddle bone deformity or other problems like arthritis or injury to tendons and ligaments around this joint area (which may also be responsible for some pain).
Identifying the Causes
In order to identify the cause of your saddle bone deformity, it’s important to consider all of the possible factors. The most common causes are:
- Excessive weight. A heavy body puts strain on your joints, especially those in your lower back and pelvis. If you’re overweight or obese, this can lead to pain in the sacroiliac joint (SIJ) area between your spine and pelvis–a common source of SDA symptoms.
- Genetic factors. Some people are more likely than others to develop SDA because their bodies have less flexibility in their connective tissue structures like ligaments and tendons; this makes them more susceptible to injury when they’re active or doing physical labor that involves repetitive movements such as running while carrying heavy loads over long distances at high speeds like soldiers do during combat training exercises where they carry full gear packs weighing up to 100 pounds each!
Osteoarthritis and Bone Spurs
Bone spurs, or osteophytes, are bony growths that can cause pain and stiffness in the joints. They’re usually caused by osteoarthritis–the breakdown of cartilage that cushions the ends of bones within a joint.
Osteoarthritis is most common in older people who have had repeated trauma or overuse injuries to their joints over time. It’s also associated with obesity, smoking and genetics (you may be more likely to develop it if your parents had it).
Other Contributing Factors
Other contributing factors to saddle bone deformity include:
- Genetic predisposition. A person with a family history of saddle bone deformity is at a higher risk of developing the condition themselves, though it’s not guaranteed.
- Injury to the bone. This can occur from an accident or injury, such as falling off a bicycle or tripping over something on the ground while running outdoors. In some cases, repetitive stress injuries (like those sustained by athletes who play sports) may cause damage to the joint and contribute to saddle bone deformity over time if left untreated for too long before seeking medical attention for it.
- Joint degeneration and osteoarthritis are common causes of this condition in older people who have been diagnosed with arthritis in their lower limbs due to age-related wear and tear over time — meaning that as you get older, there’s more chance you’ll develop symptoms like these than someone younger than yourself who hasn’t been exposed yet! However…
Common Symptoms
A discomforting lump, a sharp irritation, or a burning sensation at the top of your foot often gives away the presence of this condition. Pain and discomfort in the area.
- Swelling
- Tenderness
- Bruising
- Increased movement in the joint, which may be felt as grinding or popping sounds when you move your horse’s leg. This increased movement can cause damage to other tissues and tendons around your horse’s knee, causing further problems.
- Loss of function due to pain
It’s almost as if our foot speaks its own language and these are its cries for attention!
Diagnosing and Treating Saddle Bone Deformity
If you’re considering surgery, it’s important to know that there are several options. The choice you make will depend on the severity of your deformity and what kind of activity you want to be able to do after treatment.
- Surgery: In this procedure, called osteotomy (or bone cutting), the surgeon breaks part of the bone and moves it into a new position so that it fits better in its socket. This can be done using metal plates or wires during surgery or by putting them in after surgery with screws or pins that go through soft tissue only (therefore avoiding damage).
- Non-surgical treatments: These include exercises aimed at strengthening muscles around joints, wearing an orthotic device such as an AFO brace on one foot only while walking for balance support until both feet can be equally supported without being braced; using crutches when needed for stability until full recovery occurs; icing sore spots regularly throughout each day; elevating legs above heart level whenever possible during daytime hours while lying down–especially if swelling has occurred due to inflammation caused by arthritis flares over time due lack circulation problems causing fluid buildup inside thighs due lack blood supply flow caused by poor circulation stemming from lack muscle tone resulting poor circulation quality control leading ultimately deterioration over time
Diagnosing Saddle Bone Deformity
To diagnose saddle bone deformity, your doctor will ask about your symptoms and perform a physical examination. Your doctor may also order tests to help determine the cause of your pain.
The doctor will also consider your medications and lifestyle when making a diagnosis. If you’re taking drugs that suppress the immune system or have recently had surgery, those may be contributing factors to the problem in question.
Medical Examination
If you suspect that you or your horse has a saddle bone deformity, consult with your veterinarian. He or she will perform a thorough physical examination of the affected area and may also want to examine other parts of your horse’s body. The following is an overview of what to expect during this process:
- Examine the affected area for redness, swelling and pain (signs of infection).
- Check for tenderness around bones and joints (signs of inflammation).
- Determine if there are any deformities in other areas of the body that could be related to this condition (for example, crooked legs).
Diagnostic Procedures
Once you’ve been diagnosed with saddle bone deformity, your healthcare provider will likely perform several diagnostic procedures. These tests can help determine the cause of your condition and how best to treat it.
Some of these tests include:
- X-rays. This test uses low-dose x-rays to create images of internal structures in the body. It’s often used to diagnose broken bones or other skeletal problems such as arthritis or osteoporosis (thinning of the bones). In some cases, an MRI may be recommended instead of an X-ray if there are concerns about exposure to radiation from too many x-rays over time; however, MRIs aren’t always available at all hospitals and clinics so they may not be accessible right away when needed most urgently by someone who has just been diagnosed with saddle bone deformity
- Physical exam. During a physical exam, your doctor will check you for signs of saddle bone deformity and other skeletal problems that may be causing or contributing to the condition. Your doctor will also ask about your medical history and lifestyle habits such as riding horses as part of this evaluation. They may also perform additional tests depending on what they discover during the initial exam.
- Blood tests. Blood tests are often used to help diagnose a variety of conditions including saddle bone deformity. In some cases, your doctor may recommend that you have certain blood work done before physical therapy or other treatment options can begin; however, this isn’t always necessary so be sure to ask if any additional testing is necessary before agreeing to it.
Treatment Options
The best treatment option for saddle bone deformity depends on the severity of your condition and individual circumstances. Options include:
- Non-surgical treatments. In mild cases, your doctor may recommend a compression sleeve or brace to help stabilize the joint and reduce pain. You can also try physical therapy exercises such as stretching and massage, which may help relieve discomfort associated with this condition.
- Surgical treatments. If non-surgical options aren’t working well enough for you, surgery may be necessary in order to correct any damage done by saddle bone deformity or prevent further damage from occurring in future years as you age (though some people choose not to undergo surgery). Surgery options include:
Non-Surgical Treatments
There are several non-surgical treatments available to treat saddle bone deformity. These include:

- Exercise. Regular exercise is important for maintaining healthy bones, especially as you age. The best types of exercises for your bones are weight-bearing ones that involve your legs and feet (such as walking, jogging or cycling). If you have limited mobility in the affected area due to pain or other factors, try swimming instead because it helps strengthen muscles without putting pressure on damaged joints.
- Massage therapy may be helpful if you have signs of inflammation such as swelling around the joint capsule (the outer layer surrounding a joint). This can relieve pain while improving blood flow through increased tissue flexibility and reducing stiffness caused by excess scar tissue formation at injured sites within muscles or tendons near affected areas; however it should only be used under professional supervision since massage therapists often use deep pressure techniques which could potentially cause further injury if not performed properly
- Medications. Nonsteroidal anti-inflammatory drugs (NSAIDs), such as aspirin, ibuprofen and naproxen can help reduce pain and inflammation caused by arthritis. Some NSAIDs may also slow cartilage breakdown in joints.
- Corticosteroid injections. These are often used to treat inflammation, swelling and stiffness in chronic joint conditions such as rheumatoid arthritis. Corticosteroids may be injected directly into the affected joints or given intravenously (IV) in case of a systemic reaction. They can provide temporary relief from symptoms but they don’t address the underlying causes of arthritis, so they shouldn’t be used for more than three months at a time without consulting your doctor first.
- Steroid injections may also be used to treat other types of joint pain, such as bursitis or tendonitis. However, they should only be given by a qualified medical professional since there are some side effects associated with their use.
- Diet. A healthy diet can help reduce some of the symptoms associated with arthritis, such as pain and stiffness.
Surgical Treatments
If you need surgery, your doctor will decide which technique is best for you. The goal of surgery is to remove the extra bone and relieve pain.
One method of removing the saddle bone involves cutting through the skin and muscle overlying it, then pushing apart and pulling up on each side of your tailbone until you can see where it attaches under your pelvis. The surgeon uses special surgical instruments called osteotomes (sharp chisels) or rongeurs (screwdrivers) to cut off this attachment point from below so that only one piece remains attached at its top end–this piece becomes part of your sacrum after healing takes place.
The second technique involves making an incision overlying both areas where extra bone has formed around iliac crests; these incisions are made toward each other until they meet in front of pubic symphysis . Then surgeons use their hands during surgery rather than instruments; they grasp firmly onto both sides’ attachments using forceps or clamps before pulling them apart slowly until complete separation occurs without causing additional damage and bleeding into surrounding tissues due to excessive traction being applied.”
The third technique involves making an incision overlying both areas where extra bone has formed around iliac crests; these incisions are made toward each other until they meet in front of pubic symphysis . Then surgeons use their hands during surgery rather than instruments; they grasp firmly onto both sides’ attachments using forceps or clamps before pulling them apart slowly until complete separation occurs without causing additional damage and bleeding into surrounding tissues due to excessive traction being applied.
Preemptive Measures and Management
To prevent saddle bone deformity, you should avoid strenuous activities that put pressure on your saddle bone. These include running, jumping, climbing and other sports involving sudden changes in direction. In addition to wearing proper footwear, it’s important that you sit with legs uncrossed at all times. This will help prevent pressure on your saddle bones while sitting down or lying down (for example when sleeping). Finally, maintaining a healthy weight will help ensure that nothing else puts undue stress on these bones as well keep them strong enough so they won’t break under normal use.
Preventing Saddle Bone Deformity
The best way to prevent saddle bone deformity is by avoiding repetitive stress on your feet. If you’re an athlete, consider switching up your sport or even taking up a new sport. If you don’t want to give up your favorite activity, try wearing supportive shoes that will help distribute weight evenly across all of your foot’s bones and muscles.
Additionally, be sure not to put too much pressure on any one part of your body during activities like running or lifting weights: spread out the pressure as much as possible! This can be done by bending at the knees instead of from the waist (which puts more weight on one side), or alternating which leg takes steps when walking or running so that each leg carries equal amounts of weight for longer periods of time.*
Managing the Condition Effectively
If you’re living with saddle bone deformity, it’s important to take good care of yourself. In addition to the treatments recommended by your doctor, there are some things that you can do at home to help manage the condition effectively:
- Regular exercise is key for maintaining good posture and strengthening muscles around the pelvis. Stretching exercises are especially beneficial because they improve flexibility in tight areas like hamstrings and hip flexors–two areas that often become tight due to sitting all day at work or school (or both).
- Maintain a healthy diet that includes plenty of fruits and vegetables as well as lean proteins such as poultry or fish. Avoid processed foods containing sugar or refined flour whenever possible; these types of ingredients tend not only increase inflammation but also contribute excess calories without any nutritional value whatsoever! * And lastly but most importantly: avoid high impact activities such as running which could further damage already weakened joints!
Saddle bone deformities can be treated.
There are several treatment options available for saddle bone deformity. If you have the condition, your doctor can prescribe medications or perform surgery to help improve the alignment of your bones and prevent future problems.
If you’re concerned about saddle bone deformity, it’s important to talk with your doctor about how this condition affects your overall health. Your doctor will likely recommend exercises designed specifically for people who have a mild form of this condition as well as activities that promote good posture and balance (such as yoga). In addition, they may recommend wearing shoes with higher arches or custom orthotic devices inside them so that they provide extra support while walking around all day long!
Conclusion
In conclusion, it’s important to understand that saddle bone deformities are manageable and treatable. With the right treatment plan and care, you can manage your condition and prevent future complications from occurring.







